Three-year Outcomes of the Post-Approval Study of the AtriCure Bipolar Radiofrequency Ablation of Permanent Atrial Fibrillation Trial
The Evidence Is In and Has Been for Years: How The ABLATE Studies Set the Standard and Hold Strong Where it Counts.
McCarthy, P.M. et al. (2022). J Thorac Cardiovasc Surg. doi:10.1016/j.jtcvs.2020.09.099
Introduction
The prospective, multicenter, single arm ABLATE post approval study (PAS) led by Patrick M McCarthy and colleagues (Division of Cardiac Surgery, Northwestern University Feinberg School of Medicine, Bluhm Cardiovascular Institute, Chicago, Illinois) evaluated long term outcomes of patients with preexisting atrial fibrillation (AF) who were treated with the Cox Maze IV (CMIV) procedure.1
Methods
A total of 365 patients, with a pre-procedure mean AF duration of 60.0±84.2 months (0.3% paroxysmal, 56.7% persistent and 43% longstanding persistent atrial fibrillation), enrolled between June 2010 and October 2014 at 40 centers, underwent the CMIV procedure using the Isolator® Synergy™ Clamps (AtriCure, Inc., Mason, Ohio). The primary effectiveness endpoint was determined as the proportion of patients who were free from AF (defined as AF, atrial flutter or atrial tachycardia episodes >30 seconds in duration) while off class I and III antiarrhythmic drugs (AADs) for at least 4 months (except amiodarone which was stopped 12 weeks before evaluation) at 1-, 2- and 3-years post-procedure. The primary safety endpoint was the proportion of patients who experienced a serious device or ablation procedure-related adverse event excluding the need for a pacemaker within 30 days of the index procedure or hospital discharge. Data were adjudicated by an independent clinical events committee. A pre-performance safety goal expected that 47.8% of patients would achieve freedom from AF. Occurrences of AF lasting >30 seconds in duration were documented using a 48-hour Holter monitor, Zio Patch, or permanent pacemaker interrogation recording performed at each yearly follow-up.
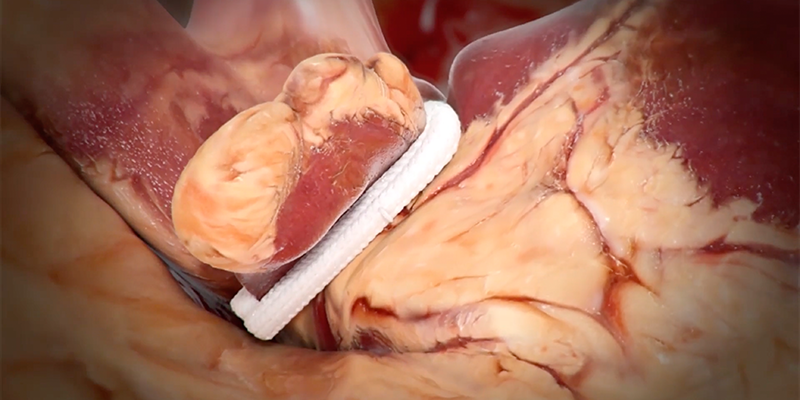
Cox-Maze IV Lesion Set
In brief, left and right pulmonary vein isolation (PVI) followed by ablation to the roof and inferior lines were conducted to create a box lesion. Additional ablation lines were performed at the mitral valve annulus, connecting lesion from the left atrial appendage (LAA) to the left PV lesion. Right atrial lesions from atriotomy to tricuspid valve annulus, ablation of the superior and inferior vena cava were recommended but not mandatory. Right-side lesions at the right anterior free wall appendage and right atrial appendage to annulus and left side lesions at the LAA could be performed but were considered optional.
Results
A total of 343 (94.5%) of patients underwent a full bi-atrial CMIV whereas 14 (4%) did not have right atrial lesions. Most patients (82%) underwent a concomitant valve operation with CMIV. There were no serious device events within 30 days of the procedure or index hospitalization, however 1.1% (4/365) experienced a serious ablation procedure event. Mortality occurred in 5.5% (20/365) of patients with respiratory failure as the most common cause. Other adverse events included excessive bleeding in 1.9% (7/365), stroke in 1.6% (6/365), myocardial infarction in less than 1% (3/365) and new permanent pacemaker implantation in 15.2% (50/329) at the index hospitalization and in 23.7% (78/329) throughout the trial.
A total of 82.1%, 72.2% and 67.2% of patients completed the 1-, 2- and 3-year follow-up visits, respectively. Primary effectiveness off AADs at 1-, 2-, and 3-years was 66.2% (95% CI, 60.3-71.7), 64.9% (95% CI, 58.6-70.9) and 64.3% (p<0.0001; 95% CI, 56.4-69.2) (Table 1). The observed primary success rate at 36 months was significantly higher than the pre-established performance goal of 47.8% (P<0.001).
ABLATE IDE Trial
For comparison purposes, the former AtriCure Bipolar Radiofrequency Ablation of Permanent Atrial Fibrillation (ABLATE) investigational device exemption (IDE) trial demonstrated that the CMIV procedure performed with the AtriCure Isolator Synergy Clamps (AtriCure, Inc., Mason, Ohio) was safe and effective for patients with persistent or long-standing persistent AF who underwent concomitant cardiac surgery. A total of 76% of patients off AADs were AF free at 6 months post-procedure (Table 1).2
Table 1. Comparison of Results Between the ABLATE IDE Trial and ABLATE Post Approval Study
| ABLATE IDE | ABLATE Post Approval Study | |||
|---|---|---|---|---|
| Follow-up period | 6 months | 1 year | 2 years | 3 years |
| Freedom from AF off AAD, % (n/N) | 76% (38/50) | 66.2% (184/278) | 64.9% (159/245) | 64.3% (146/232) |
| Freedom from AF on/off AADs, % (n/N) | 84% (42/50) | 79.7% (216/271) | 77.8% (187/242) | 75.6% (168/228) |
AAD=antiarrhythmic drug. Episodes of atrial fibrillation (AF) were defined as those lasting longer than 30 sec in duration.
Key Takeaways
- Use of a standardized CMIV procedural approach to treating patients with preexisting AF who underwent
concomitant cardiac surgery demonstrated robust, durable lesions through 3 years of follow up with an
average continued freedom from AF of 64.3% off AADs and 75.6% on or off AADs. - Results of this post approval study and those from the ABLATE IDE Trial support the Class I
recommendation for concomitant AF ablation in patients undergoing cardiac surgery.